 Over the past several years I have focused on empowering patients both with education and real-time biofeedback. In our office, we have embraced the use of remote monitoring, including an array of tools from home sleep studies, to continuous glucose monitors (CGMs).
Over the past several years I have focused on empowering patients both with education and real-time biofeedback. In our office, we have embraced the use of remote monitoring, including an array of tools from home sleep studies, to continuous glucose monitors (CGMs).
After reviewing over 10,000 CGMs, I wanted to share some of the lessons/insights that I have learned from my patients and their CGM readings. Here are 8 key lessons.
Lesson 1: Hidden carbs are everywhere
You will find hidden sugar & carbs everywhere. You thought that the steak you were eating at a restaurant had no sugar, but they slid it into the sauce or the rub. Oftentimes, even when you ask the waiter when you dine out, they will claim that “there is no sugar” but your CGM will tell you a different story. Low-and-behold, that dish had agave, or honey, or maple syrup which are all sugar by another name!
You will also find that other items you didn’t think had carbohydrates actually sometimes have more than you’d expect. Hotdogs, sausage, beef jerky, grilled chicken bites, spices, condiments, sauces, soups, broths, basically everywhere you didn’t look, have carbs!
Lesson 2: Consider avoiding seed oils, and vegetable oils, especially from restaurants.
For reasons I cannot completely yet explain, many of my patients have reported that fried foods will increase their blood sugars.
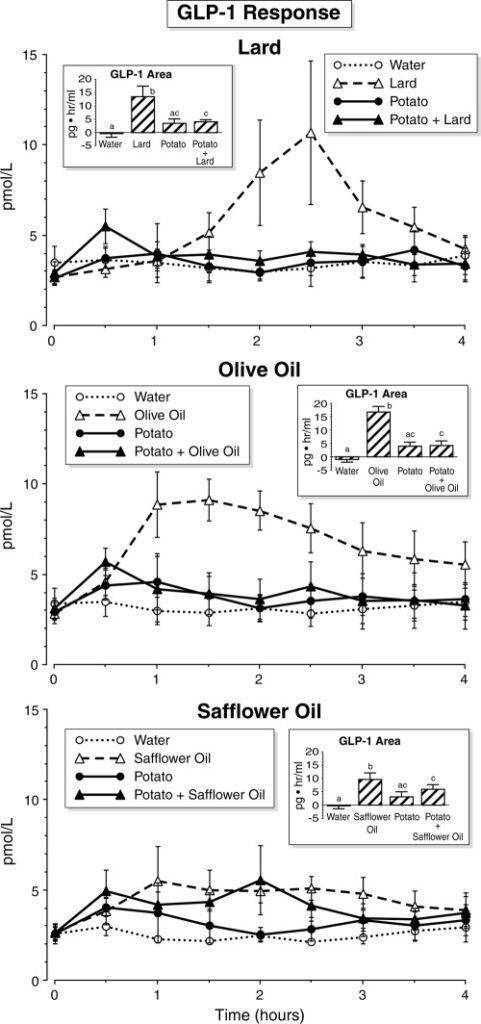
In my search to explain these findings, I came across a study that showed that these oils appear when combined with carbohydrates cause a relatively decreased release of GLP1, a potent weight loss and anti-diabetic incretin hormone.
Patients who report a switch to olive oil and avocado oil & good old-fashion home cooking seem to have improvements on their CGM that are not otherwise explainable.
Lesson 3: Don’t combine carbs and fat
The combination of carbs and fat in food has consistently led to my patients eating more than they want. This carb+fat signature is seen commonly in nuts, dairy, and basically all modern-processed foods. This combination leads to more dramatic blood glucose readings than carbohydrates alone. For example, many of my patients will not see an increase in their blood sugar with a small starchy vegetable, but if they take that starchy vegetable and fry it in some proceed seed oil, this seems to drive up glycemia, even if the overall amount of food/carbs are kept low. Eliminating foods that combine carbs and fat has consistently been shown to decrease glycemia on CGMs in my practice. Look to replace carb/fat combo foods with more satiating foods like meat, fish, chicken, eggs, etc.
Lesson 4: Don’t eat late
Eating late at night is associated with higher glycemia the entire next day. This could be in part to the effects of eating late on our circadian rhythms. It could also be due to the fact that sleep disturbance and less sleep duration occur with late-night eating. It could also be because 100% of binge eating happens at night. Whatever the cause, sleeping is better than eating for glycemia!
Lesson 5: Get good sleep
If sleep is disrupted due to sleep apnea, poor sleep duration, or poor sleep quality, this has been consistently shown to negatively affect the blood sugar of my patients. Improving the duration and the quality of sleep often involves decreasing electronics, decreasing blue light, as well as creating a cool and calming space for your nightly rest. It’s worth it to improve your blood sugars.
Lesson 6: When stressed out, go for a walk
Whether your body is experiencing stress from waking up in the morning or whether you are stressed due to your boss or your relationship, go for a walk! Stress hormones will increase your blood sugar without any food, this can occur daily during the early AM hours which can be seen on a CGM with increasing morning blood glucose numbers. This is called the dawn phenomenon and is associated with those natural stress hormones that can elevate blood sugars. If you see your blood sugar rise from these stress hormones, consider going for a walk. Walking, particularly in nature has been shown to decrease cortisol, improve blood sugar right away, and increase fat oxidation. Get your walk on!
Lesson 7: Do intense exercise
Although exercise modalities like resistance training (RT), metabolic conditioning (MetCon), and high-intensity interval training (HIIT) cause an initial rise in glucose, your blood sugars will decrease over the next 12-24 hours. Don’t fear that small glucose spike, get some all-out intense exercise in.
Lesson 8: Patient Empowerment
Many have asked me “what the magic of a CGM is” and the answer is simple, it is NOT magic. The magic happens when a doctor and a patient bond with a personalized approach to nutrition when doctor and patient explore their unique physiology and lifestyle issues. The CGM can be a window into a patient’s life and an opportunity to provide directed feedback but more importantly the ability for the patient to see how their life choices affect their own health. When the patients gain insight and control, the sky is the limit. If patients are given dogma and paternalism, expect poor results.
Final Thoughts
The CGM is a valuable tool, in our practice and is recommended for nearly every patient with pre-diabetes and diabetes and often for anyone who is looking for more insight into their own health. We believe in democratizing metabolic health and empowering patients with knowledge and access to care. The CGM is only the tip of the iceberg when it comes to remote monitoring. We have many more tools in our arsenal that make medicine easy, real-time, and accessible. The end results will be better patient outcomes and increased patient satisfaction.
If you are interested in getting a CGM or patient-centered metabolic care, sign up for our virtual metabolic care program (here).






